Affecting nearly 55 million people in North America alone, osteoporosis is among the most common chronic musculoskeletal disorders in the US and worldwide. This condition causes the bones to become brittle and weak, exposing patients to fractures and disability.
Osteoporosis is a “silent” disorder, meaning that its symptoms are not immediately noticeable or outwardly visible, making this condition difficult to diagnose and treat. In turn, you may only receive a diagnosis after a fracture or when your bone structure has been irreversibly compromised.
But you no longer need to live with chronic pain, endure the side effects of medications, and deal with recurring fractures. With adequate lifestyle changes Neurofunctional Pain Management, you can regain control over your health without medications or invasive procedures. Learn more below.
What Is Osteoporosis?
The word “osteoporosis” derives from the Greek terms for bone (“osteon”) and small opening passageway (“poros”). This medical term describes a condition that causes the bones to lose mass and become brittle and weak.
To understand how osteoporosis develops, it is important to clarify that the bones are not static but dynamic and living bodies that change constantly and undergo what’s known as “bone metabolism.”
Bone comprises minerals (i.e., calcium) that are kept together by collagen fibers and protected by an outer shell known as cortical bone. At a microscopic level, this structure gives bones a honeycomb-like appearance, which allows them to remain strong and flexible.
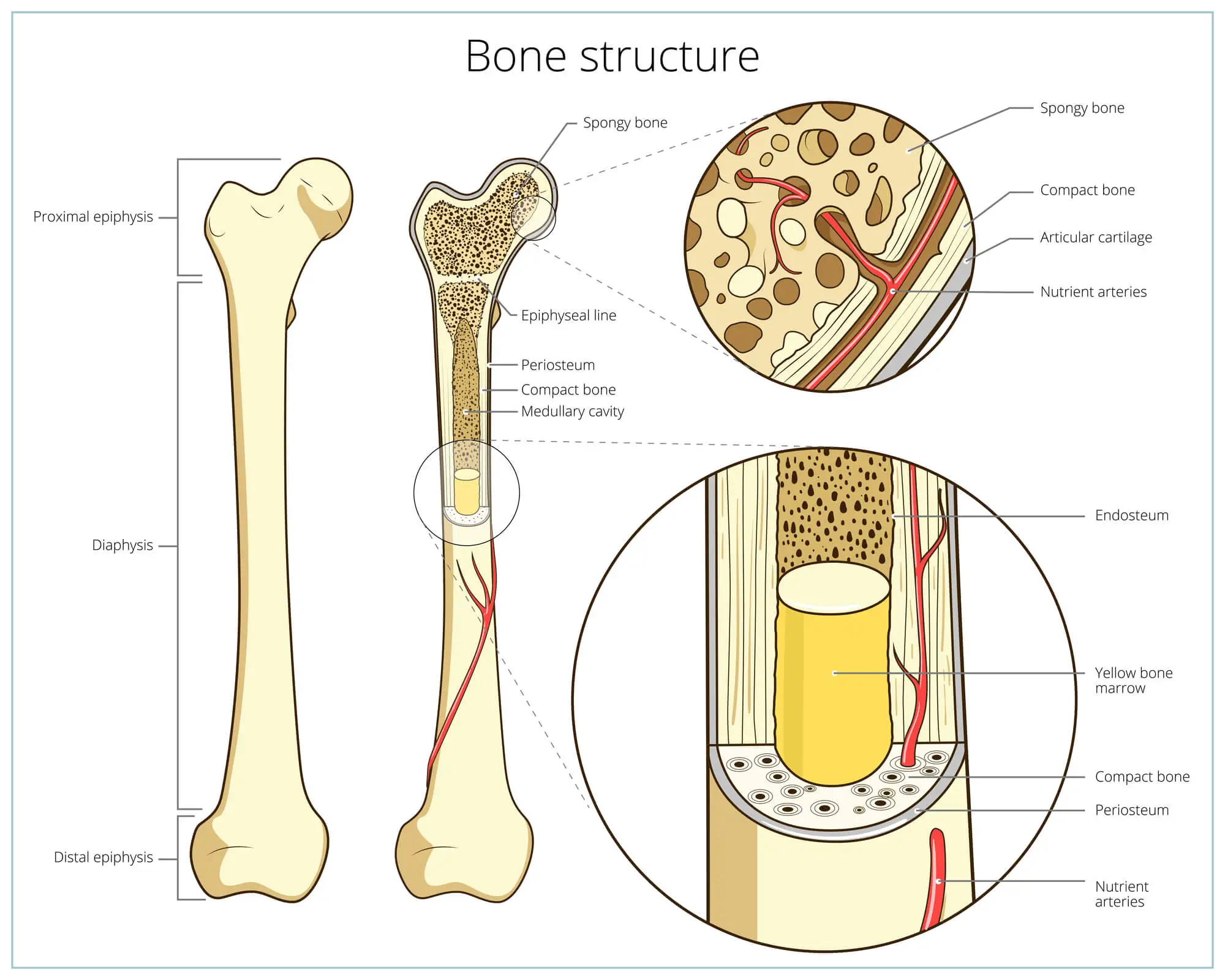
The active tissue that composes the bone continuously changes and renews itself throughout life. Cells known as osteoclasts proceed to break down old tissue and regulate the rate at which bone mass is lost.At the same time, cells known as osteoblasts produce new bone material.
The speed at which bone is formed and broken down (resorption) changes throughout life:
- During the development period (childhood and adolescence) new bone material is formed quickly and at a higher speed. The bones reach peak density by the time a person is 25-30 years old.
- To maintain balance, the adult skeleton will produce bone at the same rate at which bone mass is lost. The skeleton is entirely renewed every 7-10 years.
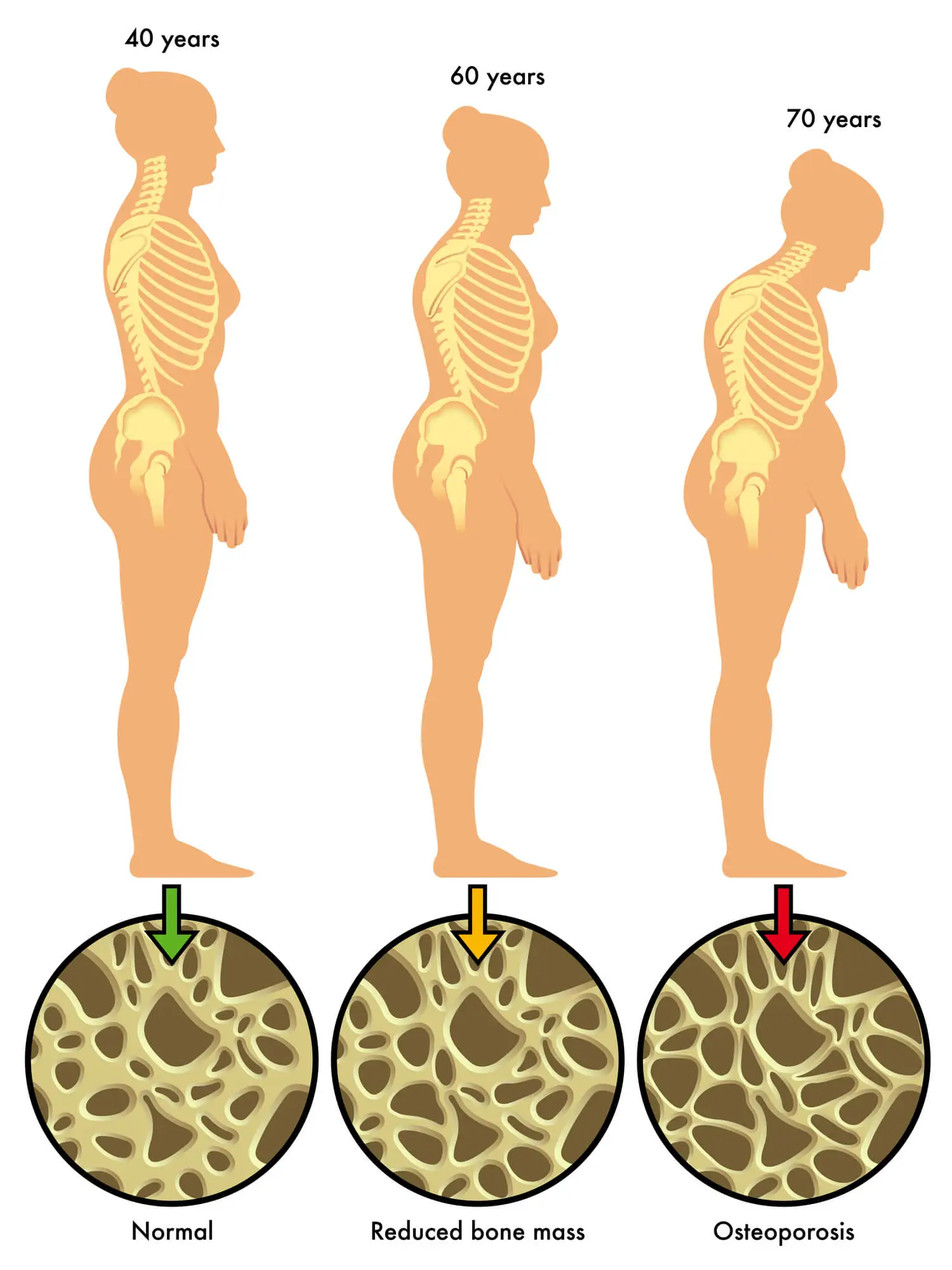
- After age 40, the bone material breaks down faster than it can be replaced. In women, 10-20% of bone mass is lost during the first 5-6 years of menopause. This means that, with aging, every person experiences bone mass loss to a certain extent.
Nonetheless, in some people, the rate at which bone mass and minerals break down is much faster than the rate at which it is replaced.
This causes the bones to lose density and the holes in the “honeycomb” to become much larger. In turn, this translates into bones that are brittle, more fragile, and prone to fracture. In people with osteoporosis, a broken bone can be caused by minimal stress, such as coughing or bending.
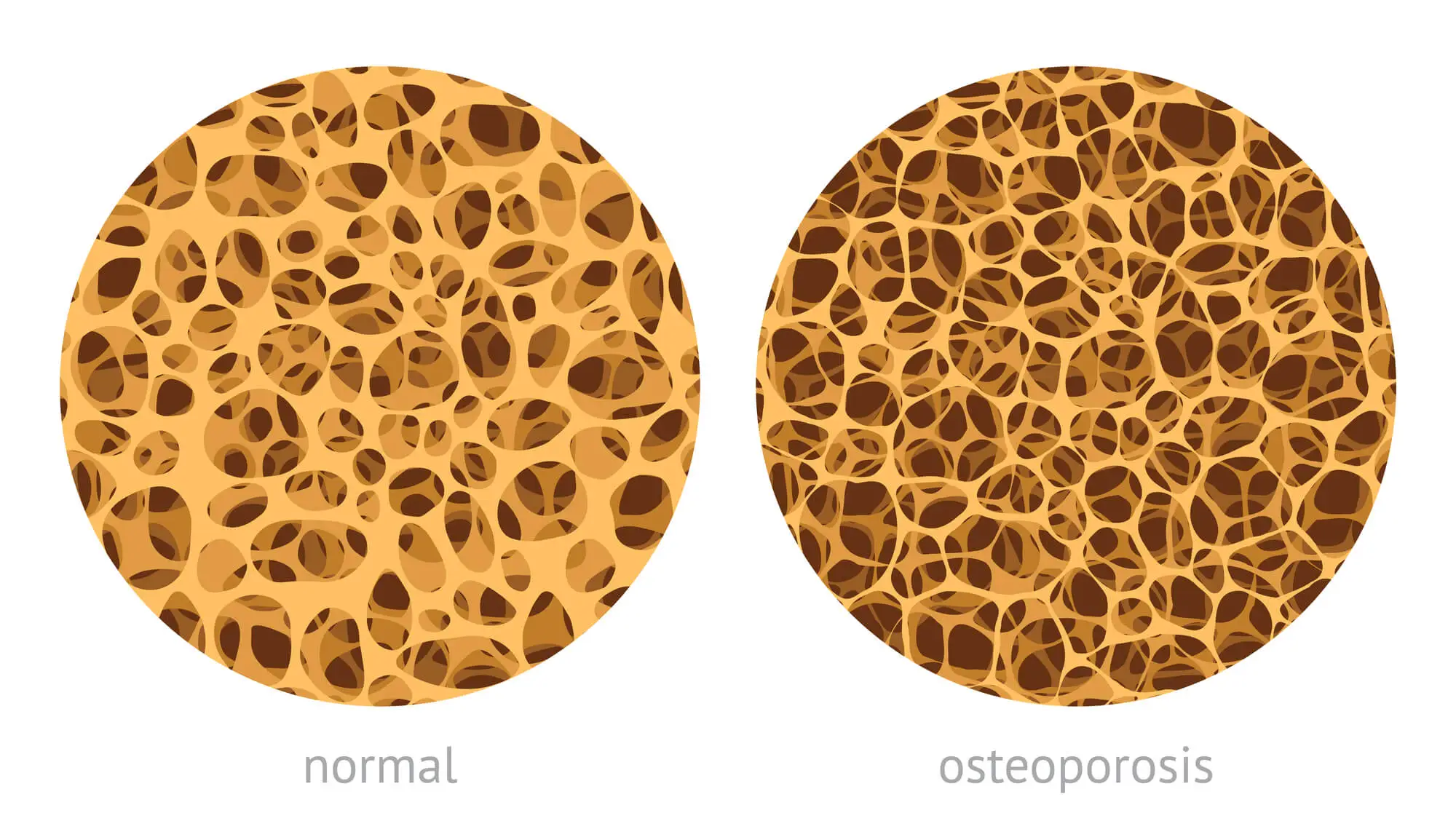
This disease develops without symptoms, and most patients only receive a diagnosis of osteoporosis when looking into the causes of a bone fracture.
Every year, osteoporosis causes over 2 million broken bones, but 80% of patients are not screened for this disease. However, learning more about this bone condition and finding adequate treatment is essential to safeguard your musculoskeletal health. Learn more below.
Types Of Osteoporosis
Although osteoporosis is more common in aging individuals, this condition can affect anyone. There are different types of osteoporosis, depending on the symptoms it causes and the demographic it affects. Let’s look at them below.
Primary Osteoporosis
Primary osteoporosis is the most common form of this condition. Primary osteoporosis is subdivided into senile osteoporosis and menopausal osteoporosis, depending on whether it is triggered by age-related bone mass loss or hormonal changes (such as those occurring during menopause). It is estimated that 1 in 2 postmenopausal women may have osteoporosis to some extent.
If the cause of primary osteoporosis is unknown, this condition is known as idiopathic osteoporosis.
A person’s bone mass throughout life determines the risk of developing primary osteoporosis in later life. Still, factors such as diet, health, physical exercise, and lifestyle may also have an impact. Primary osteoporosis is commonly diagnosed in individuals aged 60 and over.
Secondary Osteoporosis
Secondary osteoporosis is a severe and progressive loss of bone mass caused by another underlying disease. It can occur at any age. Medical conditions that can cause secondary osteoporosis include leukemia and hormonal disorders such as hyperthyroidism.
Some medications can also speed up the loss of bone density. These include high-dose corticosteroids (when taken regularly, orally or inhaled), hormone replacements, and some cancer drugs.
Osteogenesis Imperfecta
Also known as brittle bone disease, osteogenesis imperfecta is a rare genetic or heritable disease that causes bones to break easily and without obvious cause. This condition is often seen in newborns and can lead to severe complications, including a shortened lifespan. Only around 1 in 20,000 people is affected by osteogenesis imperfecta.
Idiopathic Juvenile Osteoporosis
Idiopathic juvenile osteoporosis is a rare condition that affects children and young adults, usually within the development period (8-14 years old). Although it is more common in individuals with a history of being overweight in childhood, there is no known cause or cure for this disease.
Where Does Osteoporosis Commonly Occur
Any bone in the body may be affected by osteoporosis, which can start anywhere and not cause fractures for several years. However, some bones are more prone to breaking than others.
In particular, osteoporotic fractures tend to occur in the wrists, hips, spinal bones (vertebrae), and knee. These bones or joints are usually load-bearing or exposed to constant stress, which makes them more likely to break.
If you experience a fracture in any of these bones, your doctor may prescribe a diagnostic test to assess your bone mass density and identify the signs of osteoporosis.
Symptoms of Osteoporosis
As seen above, osteoporosis is known to be a “silent” disease. Since it does not cause pain or discomfort, most patients only find out about their condition through tests performed after breaking a bone.
However, being aware of some of the telltale signs of osteoporosis may help you prevent a fracture and obtain a timely diagnosis. Let’s look at these signs below.
Fractures
Fractures are the main symptom of osteoporosis. Osteoporotic fractures can occur spontaneously (without a cause) or as a consequence of minor and normal stresses. If you suffer from osteoporosis, you may experience a fracture due to a minor fall, when coughing, or during lifting and bending motions.
Despite the efforts of the U.S. Preventive Services Task Force to increase the rate of screening tests, under 13% of patients considered to be at high risk of osteoporosis (i.e.: aging adults and menopausal women) are tested for low mineral density before a bone is broken.
Osteoporotic fractures are also the main cause of all other symptoms of osteoporosis, which we’ll see below.
Back Pain
When osteoporosis affects the bones of the spine, the vertebrae become weaker and compressed. This can lead to severe and chronic back pain, as well as reduced spinal flexibility. You may also suffer back pain if you have suffered a fracture in your spinal bones.
Abnormal Curvature Of Spine
Changes in the bone structure of the spine translate to abnormalities in your posture. Compression of the vertebrae, combined with the effects of gravity, may cause you to assume a stopped or hunched posture, which is known as “dowager’s hump” or kyphosis.
Poor posture can lead to a cascade of complications, including alteration of vertebral mechanics, low back pain, and reduced flexibility. What’s more, an abnormal curvature of the spine may reduce your lung capacity and lead to shortness of breath.
Spine problems can also be complications of osteoporotic fractures in the vertebrae.
Loss Of Height
As the vertebrae in the spine or the hip bones lose density and compress, they become weaker and prone to collapse. This, coupled with the hunched posture caused by osteoporosis, can cause a loss of height (usually 0.5-2 inches).
Pain In The Lower Back And Legs
Lower back pain can extend beyond the back itself and affect both the gluteal muscles and the many muscles of the legs. This typically occurs as a result of nerve irritation or compression in the lumbar region. When the nerves of the lower back become...
Back Pain
Back pain is an awful problem that many individuals have encountered. It has the potential to restrict normal mobility and functionality, significantly impacting a person’s quality of...
Loss Of Movement In Lower Body
Conditions that cause chronic pain can cause severe damage to important components of the joints, thus limiting your ability to move freely. For example, in patients with arthritis, the sustained high levels of inflammation degrade the joint’s cartilage,...
Joint Pain And Swelling
Joint pain is arguably one of the most common musculoskeletal complaints among adults of all ages. But the fact that this condition is so widespread does not mean that it isn't life-limiting, or that it should be overlooked. Joint pain and swelling can cause...
Lower Back Swelling Or Redness
Low back pain is one of the most common and impactful musculoskeletal disorders. According to a study published by The Lancet Rheumatology in June 2023, low back pain affects nearly 620 million people globally and represents the leading cause of years lived...
Causes Of Osteoporosis
Osteoporosis occurs when bone minerals break down faster than they are replaced. This causes the “holes” in the honeycomb-like structure of the bone to become larger and more frequent, which can compromise the stability and strength of the bone structure as a whole.
Although this process is well-understood by doctors and physicians, the reasons why some people lose more bone density than others are not always clear.
Certainly, age plays a critical role: even in healthy individuals, 10% of bone mass is lost each decade after turning 40. However, some other factors may contribute to increasing your risk of developing osteoporosis. Let’s look at these factors below.
Lack Of Calcium Or Vitamin D
Calcium is the primary component of the bones, and it plays a critical role in maintaining the bones’ health, strength, and density. On the other hand, Vitamin D is the compound that allows the body to absorb and use calcium. A lack of either of these two components can increase your risk of developing osteoporosis.
Some factors that can lead to a lack of calcium or Vitamin D include:
- A lifelong diet low in calcium
- Low calcium intake for prolonged periods
- Gastrointestinal surgery removes part of the stomach and reduces the surface area in charge of absorbing nutrients
- Severely restricting food and being underweight
- Conditions such as Celiac disease and Irritable Bowel Syndrome, damage the stomach lining and prevent the absorption of nutrients.
- Eating disorders like bulimia and anorexia, which may prevent nutrients from being absorbed
Hormonal Changes
Hormonal changes can impact bone density and health. If you have too little or too much of certain hormones, you may be at greater risk of osteoporosis.
These hormones include the following:
- Sex hormones: Sex hormones such as testosterone and estrogen help regulate bone metabolism and slow down the natural breakdown of the bone. Sex hormone levels decline with age or due to health events, such as taking medications for prostate cancer, going through menopause, or getting your ovaries removed.
- Thyroid hormones: Thyroid hormones regulate several metabolic processes in the body, including the rate at which old bone tissue is replaced. If you have an overactive thyroid, your bones may break down at a faster rate than they should.
- Overactive hormone-producing glands: Problems that affect the endocrine systems may speed up the rate at which bone density is lost.
Menopause represents a major risk factor for women because, during this health event, estrogen levels drop suddenly.
Lack Of Physical Activity
Leading a sedentary lifestyle can lead to a cascade of musculoskeletal disorders, including osteoporosis. This is because your body will compensate for a reduced muscle mass by unloading weight, stress, and shock onto the skeleton, which can result in loss of bone mass.
Practicing sports, performing weight-bearing exercises, and engaging in activities like running, walking, and dancing can restore balance and strength, thus easing the pressure on bones.
Family History Or Genetics
Some genetic and hereditary factors may contribute to your risk of developing osteoporosis:
- Family history: The presence of osteoporosis and osteoporotic fractures in a close relative (usually the mother) translates into a greater risk of low bone density problems.
- History of bone mass: The risk of developing osteoporosis is connected to the bone density you were able to achieve in your youth. Although this can depend on your diet and health, factors such as ethnicity and inherited features also play a role.
- Body frame and size: People with a small body frame or size are more likely to develop osteoporosis. This is because smaller small bones have less bone mass to draw from during the normal age-related loss of mineral density.
Other Causes
Other causes of osteoporosis include:
- Smoking: tobacco and nicotine damage the blood vessels that supply oxygen and nutrients to the bones, and inhibit the function of bone-regenerating cells.
- Alcohol use: Alcohol interferes with how the body absorbs and uses calcium, thus leading to calcium deficiencies.
- Some medications: Certain drugs impact how the body absorbs minerals and vitamins necessary to bone health, or alter the production of hormones. These medications include corticosteroids, anti-epileptics, cancer drugs, medications prescribed after an organ implant, and gastric reflux medications.
Statistics show that up to 50% of patients taking glucocorticoid (a type of steroid hormone) regularly may develop osteoporosis.
Complications Of Osteoporosis
When left unaddressed, osteoporosis can lead to a cascade of consequences. These include:
- Bone Fracture: One of the most serious complications of osteoporosis is fractures, which may occur spontaneously or frequently. Fractures to essential structures such as the hip and the spine can increase the risk of death or lead to severe disability.
- Spinal Deformities: Weakened spinal bones can cause vertebrae to collapse, thus leading to chronic back pain, deformity, and a hunched posture. Spinal fractures take over a year to heal and can cause permanent disability.
- Heart Diseases: Studies conducted in 2015 have confirmed the link between osteoporosis and heart disease. The relation is mainly due to the fact that rapid bone mass loss causes a release of calcium ions into the bloodstream, which can obstruct veins and arteries. Additionally, both osteoporosis and heart conditions are associated with sustained levels of inflammation, which affect the health of the cardiovascular system.
- Arthritis: Osteoporosis and arthritis are interconnected. Arthritis causes the loss of cartilage between the joints and results in chronic pain and reduced mobility. Both conditions are affected by inflammation and speed up the degeneration of the joints’ components.
If you are affected by regular fractures to the spine and hip, you may also experience a significant loss of work days, chronic pain, disability, and financial challenges. According to a study conducted in 2021, menopausal women, even if insured, faced the following costs in the three years after an osteoporotic fracture:
- Direct healthcare costs – between $3241 and $59,327 per year
- Indirect costs due to missed days at work and disability – between $2596 and $5848 per year.
While these complications may significantly affect your life, they can easily be prevented by obtaining an accurate diagnosis of osteoporosis early on. Let’s look at how below.
Diagnostic Procedure
Although osteoporosis is difficult to identify until a bone is broken, there are diagnostic tests that can provide patients with an accurate diagnosis of their condition. Let’s look at the methods that a doctor may use to determine your bone density:
- Evaluating The Risk Factors: A doctor will start the examination by looking at whether you are at risk of osteoporosis, such as your age, gender, underlying conditions, and medical history. They may also ask questions about previous fractures, medications you are taking, and your lifestyle (i.e.: diet, exercise, and alcohol use).
- Physical Examination: A physical exam for osteoporosis looks to identify signs that your bones are affected by low density. These include changes in posture, loss of height, balance problems, and abnormal gait. Your doctor may also assess your muscle strength and check for signs of muscle atrophy.
- Bone Density Test: One of the most efficient instruments used to diagnose osteoporosis is a bone density test. Your bone density is measured using a test known as dual-energy X-ray absorptiometry (DXA). DXA tests use X-rays to assess the mineral density of bones prone to fractures, such as the hip, spine, wrist, and knee. This test is painless and non-invasive.

If you believe that you are at risk of osteoporosis, it is important to consult your healthcare provider and undergo the necessary tests. Despite the guidelines provided by the U.S. Preventive Services Task Force, at-risk patients are seldom tested for this condition. As shown by a 2022 study, only 20% of at-risk women were screened for osteoporosis 2 years before a fracture.
Conservative Osteoporosis Treatment Option
Osteoporosis can be a life-limiting condition for which there is no definitive cure. However, if your bone density levels are still acceptable, your doctor may recommend a conservative line of treatment to prevent or reduce the symptoms of osteoporosis. These treatments often involve bed rest, lifestyle changes, and anti-osteoporosis medications.
Let’s look at these options in more detail below.
Bed Rest
Prolonged bed rest and immobilization are some of the risk factors for osteoporosis. This occurs in individuals who have suffered a stroke or serious illness and are therefore unable to practice activities that promote bone health (i.e. weight-bearing exercises).
However, in some cases, bed rest may benefit people with complications of osteoporosis. According to new studies, a period of bed rest and immobilization following an osteoporotic vertebral fracture (a broken bone in the spine) can help the weakened bone regain stability. It is important that bed rest is supervised by a specialist and coupled with rehabilitation exercises.
If you have osteoporosis but are not recovering from a fracture, your healthcare provider will take into account factors such as your gender, age, and health. They may also recommend lifestyle changes, such as:
- Being more active
- Quitting drinking alcohol and smoking tobacco
- Adjusting your diet
- Monitoring Vitamin D and calcium levels
You may also need to take measures to prevent falls and injuries, which may easily lead to bone fractures.
Anti-Osteoporosis Pharmacotherapy
Depending on how much bone mass you have lost, as well as on your gender and family history, your doctor may recommend a pharmacological treatment for osteoporosis.
When taking medications for this condition, it is important to keep in mind that drugs come with severe side effects, including joint pain, gastric ulcers, and gastrointestinal problems like nausea and heartburn.
Additionally, medications alone are unlikely to yield the expected results: you’ll still need to improve your overall lifestyle, adjust your diet, and avoid nutritional deficiencies.
Here are some of the most common medications prescribed for osteoporosis:
- Bisphosphonates and denosumab: By inhibiting the bone cells in charge of breaking down old bone tissue, bisphosphonates can help slow down the rate of bone loss. Denosumab has been shown to offer better results than bisphosphonates, while also reducing the risk of fractures.
- Hormone-based therapies: Hormone therapies include estrogen medications, testosterone replacement therapy, synthetic hormones that mimic the hormones produced by the thyroid gland, and estrogen antagonists (chemicals with estrogen-like effects). These therapies are recommended when other therapies have not worked and the bone mass loss is due to hormonal imbalances.
- Medications to rebuild bone mass: Drugs such as teriparatide and romosozumab stimulate the growth of new bone tissue while slowing down the loss of bone density.
Physical Therapy
Weight-bearing exercises, as well as strength and resistance training, are essential to bone health at all stages of life. During childhood and adolescence, these exercises can support the building of bone mass and reduce the risk of osteoporosis later in life.
After peak bone mass is reached – usually in your late 20s – exercise no longer increases bone mass. However, it can still support the musculoskeletal system by boosting muscle strength, improving balance and coordination, reducing the risk of falls, and safeguarding the supply of oxygen and nutrients to bone tissues.
If you have osteoporosis or are recovering from an osteoporotic fracture, it is important to work with a specialized physical therapist who can recommend the best exercises to strengthen your musculoskeletal system and teach you how to exercise safely or reduce the risk of injuries.
Surgical Procedure
Most osteoporotic fractures can be treated in A&E or by wearing a cast. However, if you have experienced a severe osteoporotic fracture that needs to be manipulated, you may need to undergo surgery.
Here are the types of surgical interventions available.
Vertebroplasty and Kyphoplasty
Spinal fractures caused by osteoporosis are the most common type of fractures requiring surgery. They occur when the bones in the spine weaken and collapse, thus compressing the spine.
Vertebroplasty and kyphoplasty are two surgical techniques that involve injecting orthopedic cement into the bone. This aims to restore spine height and correct posture problems caused by the collapse of one or more vertebrae (i.e. dowager’s hump/ kyphosis).
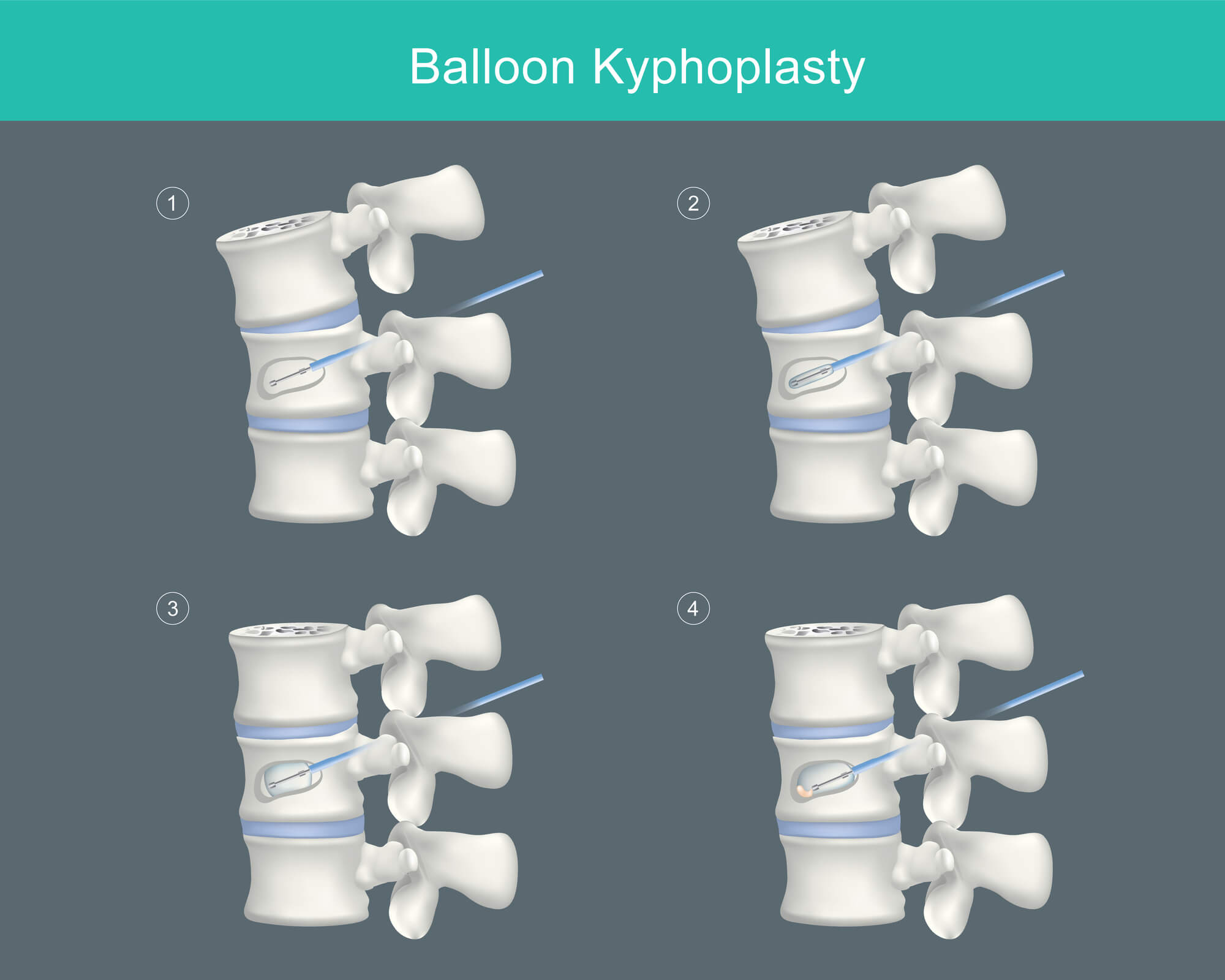
In vertebroplasty, the cement is injected directly into the fractured site, while kyphoplasty procedures use a medical device to decompress the bones and create space, before filling this newly-created void with cement.
Although these surgical procedures are sometimes necessary and often successful, they are not free of side effects. Some of the most common complications of vertebroplasty and kyphoplasty include:
- Infection: Vertebroplasty and kyphoplasty are minimally invasive procedures, but they can lead to life-threatening infections, especially among elderly and immuno-compromised patients. In a 2013 study, 3 out of 9 patients who underwent surgery showed signs of infection within a month.
- Cement leakage: Cement leakage is one of the most common complications of vertebroplasty and kyphoplasty, occurring in 18-55% of patients. This complication can be life-threatening or lead to neurological dysfunction and pulmonary embolism.
- Bleeding: Vertebroplasty and kyphoplasty procedures carry a moderate risk of bleeding. Because of this, tests to check how long it takes for a patient’s blood to clot and a complete blood count should be carried out before the procedure.
- Nerve Damage: This rare but severe complication occurs when nerves in the spinal cord are damaged during vertebroplasty and kyphoplasty procedures, or due to cement leak following surgery.
- Fracture of Adjacent Vertebrae: The decompression of collapsed vertebrae can cause fractures in adjacent spinal bones, especially if these have been weakened by osteoporosis.
Spinal Fusion
Spinal fusion is a major and invasive surgical procedure used to permanently bind the vertebrae together using screws, rods, and bone grafts. This procedure may provide support to compromised spinal bones in people with osteoporosis and can be used to correct posture problems such as kyphosis.
Some of the complications associated with spinal fusion procedures include:
- Infection: Infection represents the most common complication of spinal fusion procedures. It can occur between 3 months and 3 years after the surgery and affect up to 5% of patients.
- Blood Loss: Blood loss can be caused by a range of complications, including poor wound healing, excessive bleeding, and injury to blood vessels surrounding the spine.
- Nonunion or Pseudarthrosis: Non-union is a severe complication of spinal fusion procedures, which occurs when the spinal bones fail to bind together. This causes the rods and screws to become loose and lead to chronic pain, instability, and compromised spinal function.
- Chronic Pain: Damage and instability of the spinal column caused by spinal fusion procedures can cause chronic back pain.
- Failure to Improve Symptoms: In some cases, spinal fusion procedures fail to improve the symptoms of osteoporotic fractures. Failed back surgery can also cause chronic pain in different sites, reduced mobility, spasms, numbness, and inability to recover.
Joint Replacement Surgery
Joint replacement surgery – or arthroplasty – is a surgical procedure used to restore the function of compromised joints. During this procedure, artificial joint components made of plastic or metal are used to replace bones and cartilage. Common sites where joint replacement surgery is performed include the hips and knees.
Arthroplasty may come with severe side effects, including:
- Blood Clots: Arthroplasty can impact how the blood flows and clots around the affected site. This makes deep vein thrombosis (DVT) – or blood clots – more likely. Blood clots occur in 40-60% of patients undergoing hip replacement surgery and lead to longer hospitalization, pain, and complications like pulmonary embolism and death.
- Implant Failure: Implant failure and malfunction of the artificial joint component can occur because of wear and tear, poor installation, loosening, and dislocation. This complication can affect joint function and permanently damage nearby components of the joint.
- Fracture: Periprosthetic fractures are the breakage of the bones surrounding the artificial joint components. These can occur when the bone keeping the implant in place collapses under excessive stress. This complication is more likely among people with osteoporosis.
- Chronic Pain: Although pain after surgery is a normal part of the process, post-operative pain becomes chronic in 10% of patients. Loose implants, infections, and fractures are common causes of chronic pain.
How Neuragenex NFPM Approaches Osteoporosis
Osteoporosis is a lifelong condition, for which there is no permanent cure. Often, the treatment option recommended by your doctor will depend on your risk of breaking a bone within the next 10 years. This means that, for many, relying on medications and enduring chronic pain may seem to appear as the only options.
However, alternative treatment programs that don’t involve medications or surgery are available. With the right education and guidance, you can find treatment plans that can slow down the progress of osteoporosis, strengthen your musculoskeletal system as a whole, and magnify your quality of life.
Here are some of the therapies combined in Neurofunctional Pain Management®:
Electroanalgesia
Electroanalgesia is a pain management technique that uses high-pulse electrical current to ease pain, boost blood circulation, improve mobility, and induce...
IV Therapy
IV nutritional therapy, or intravenous therapy, involves administering vital nutrients directly to the bloodstream through an IV. This type of treatment bypasses the digestive system, allowing for maximum absorption and utilization of nutrients by the...
Lifestyle Counseling
Lifestyle counseling is an approach to managing chronic pain that involves identifying, assessing, and modifying lifestyle factors contributing to an individual's pain. For example, lifestyle factors such as nutrition, physical activity, stress, sleep quality...
Ways To Reduce Risk Of Osteoporosis
Some risk factors for osteoporosis – such as genetics and sex – cannot be modified. However, there is a lot that you can do throughout your life to reduce the risk of developing low bone mass density.
These include:
- Leading an active lifestyle and following a diet rich in calcium and vitamin D throughout your life.
- Considering taking supplements or increasing the levels of calcium and vitamin D in your diet
- Working with a specialized physical therapist to understand how to keep your musculoskeletal system healthy as you age
- Practicing strength training as well as weight-bearing and balance exercises
- Limiting alcohol and tobacco consumption
Working with a specialized lifestyle counselor and nutritionist can help you understand how to lower the risk of developing osteoporosis.
Regain Your Body’s Full Mobility With Us Today
For most patients, osteoporosis is a lifelong condition that impacts all aspects of their lives. However, taking medications daily, enduring the side effects of pharmacological therapies, or living in fear of having to undergo surgery are no longer the only options to manage your condition.
With Neuragenex Neurofunctional Pain Management, you can regain control over your bone health without medications or surgery.
We provides advanced treatments to reduce fractures and associated pain. Schedule a consultation today!